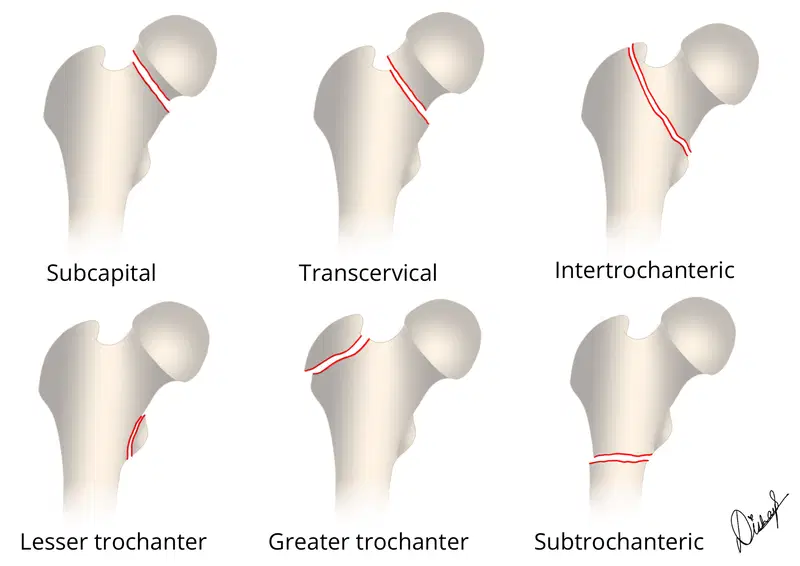
Femoral neck fractures are subdivided based on the location of the fracture, including head fractures and neck fractures including subcapital, transcervical, basicervical, intertrochanteric and subtrochanteric. These are best classified as intra and extracapsular as that dictates management.
How many of these fractures subtypes can you identify? Check the labelled image at the end of the article.
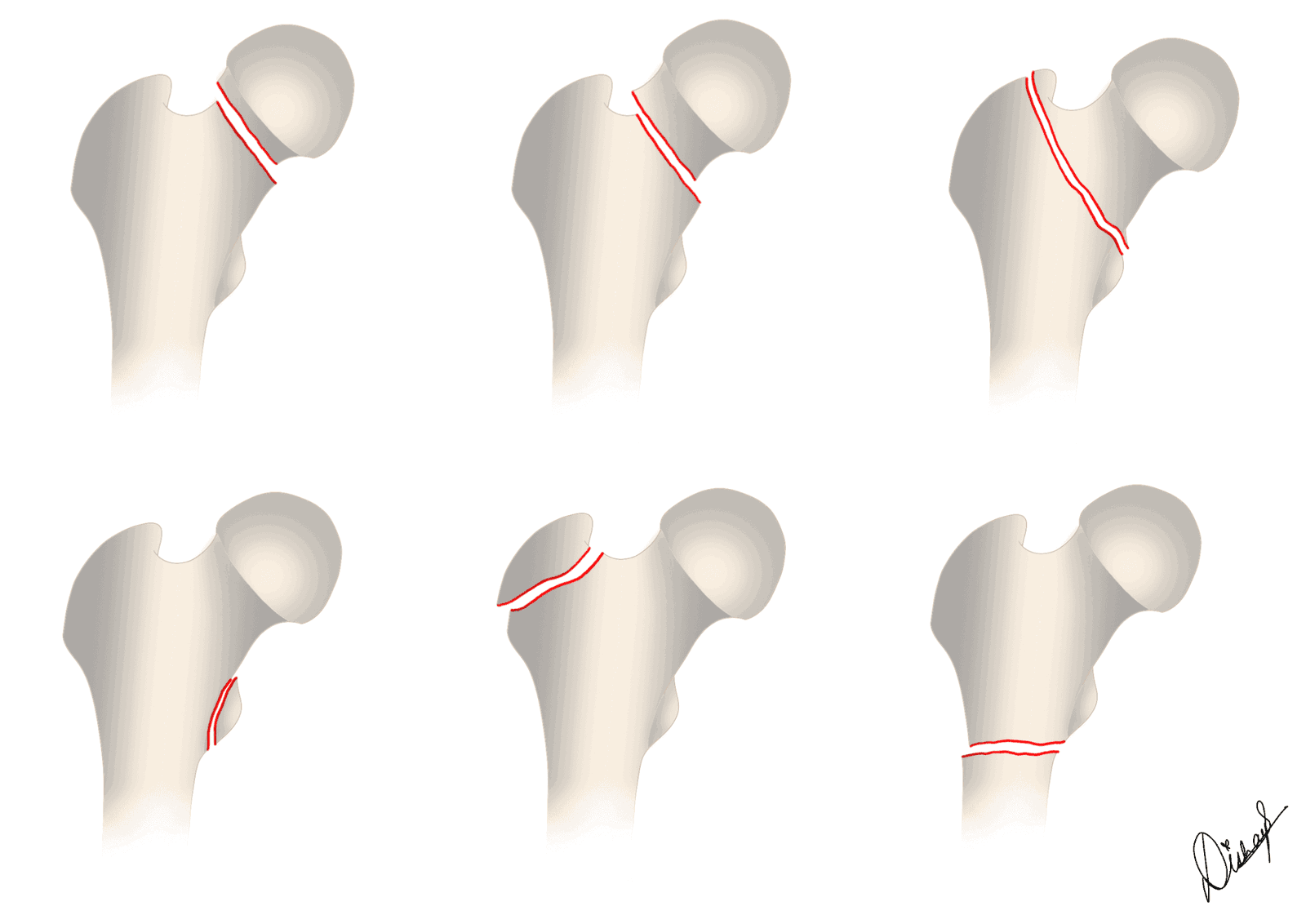
| Subtype of proximal femoral fracture | Intracapsular or Extracapsular? |
| Subcapital | Intracapsular |
| Transcervical | Intracapsular |
| Basicervical | Functionally extracapsular |
| Intertrochanteric | Extracapsular |
| Subtrochanteric (within 5 cm from lesser trochanter) | Extracapsular |
| Greater Trochanter | Extracapsular |
| Lesser Trochanter | Extracapsular. Consider pathologic fracture |
Why is it important to distinguish intra and extracaspular proximal femoral fractures?
If there was one take away point from this article, it would be this.
Intracapsular fractures in the femoral head can significantly affect its blood supply, leading to nonunion of the fracture or avascular necrosis (AVN). The lateral margin of the femoral head-neck junction is particularly important because it is where the lateral epiphyseal vessels are most commonly affected. Fractures in this area have a high risk of causing serious damage to the blood vessels, although the risk decreases as fractures occur further down the femoral neck. Treatment for fractures in the femoral head and neck must consider the potential compromise of blood flow and focus on maintaining, restoring, or replacing the blood supply to prevent these complications.
On the other hand, basicervical and intertrochanteric fractures pose minimal risk to the blood flow in the femoral head. Treatment for these fractures involves aligning the bones and stabilizing them with implants, allowing early movement and weight-bearing during healing.
Femoral head fractures are rare and often associated with dislocation and high energy trauma. These are classified according to Pipkin classification system.
Femoral head impaction fractures can be seen with anterior and posterior dislocations. A similar pattern of injury is also seen in osteoporotic patients with focal subchondral insufficiency fractures. It is important to differentiate these from avascular necrosis.
On MRI, these fractures resemble femoral head osteonecrosis, with a dark subchondral line and a larger area of bone edema. However, subchondral insufficiency fractures differ histologically from osteonecrosis, as they consist mainly of fracture callus and granulation tissue with bone edema and enhancement above and below the fracture line. In contrast, osteonecrosis exhibits devascularized bone without enhancement. Subchondral insufficiency fractures also tend to have an irregular and convex appearance compared to the joint surface, while osteonecrosis presents as a smooth, continuous, and concave dark line.
Femoral neck fractures are classified according to the Garden System in elderly patients (>70-75 years) and Pauwels system in young adults (<65-70 years)
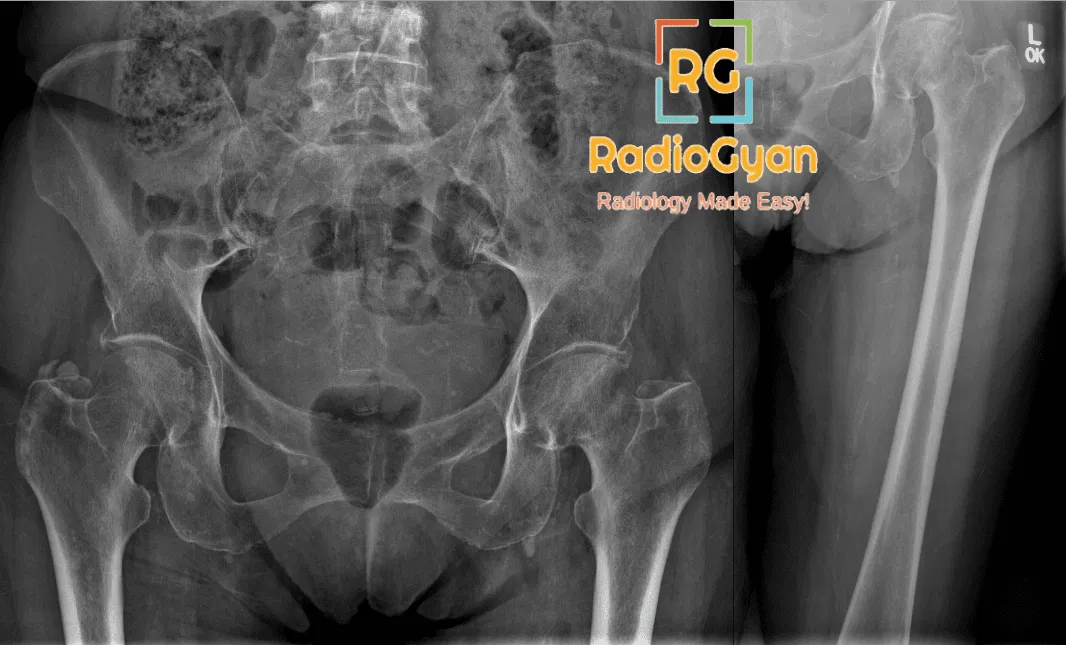
| Classification | Displaced or undisplaced? | Description | Incomplete, nondisplaced, including valgus-impacted fractures |
| Type 1 | Nondisplaced | Incomplete, nondisplaced, including valgus impacted fractures | ~7% AVN. Typically treated with percutaneous fixation |
| Type 2 | Complete, nondisplaced | ||
| Type 3 | Displaced | Complete, incompletely displaced | ~ 37% AVN. Typically treated with ORIF or arthroplasty |
Although a few basicervical fractures can be intracapsular, the incidence of avascular necrosis is low in these and they are treated as extracapsular fractures.
Extracapsular fractures are treated with open reduction and internal fixation. Evans classification system is used for intertrochanteric fractures.
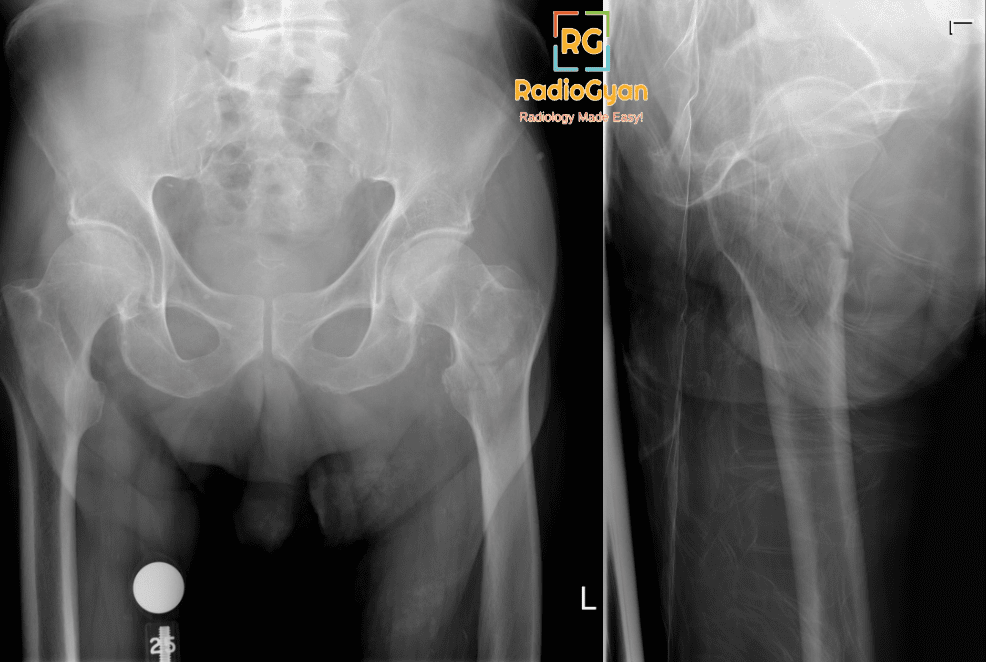
Subtrochanteric fractures are fractures within 5cm from the lesser trochanter. The Russell-Taylor system classifies these into two main types: type 1, which is characterized by the absence of piriformis fossa extension, and type 2, which indicates the presence of intertrochanteric extension.
These are seen in three scenarios:
- Younger patients, usually under the age of 50, tend to have high-energy trauma that leads to comminuted fractures.
- Elderly patients, who are more likely to have baseline osteoporosis, experience lower-energy trauma, such as falls from a standing height. This often results in less comminuted spiral fractures, which are known as “typical” insufficiency fractures.
- Patients with medical comorbidities or those receiving long-term bisphosphonate therapy (over 5 years) are at risk of stress fracture development due to impaired bone remodeling (atypical femoral fractures).
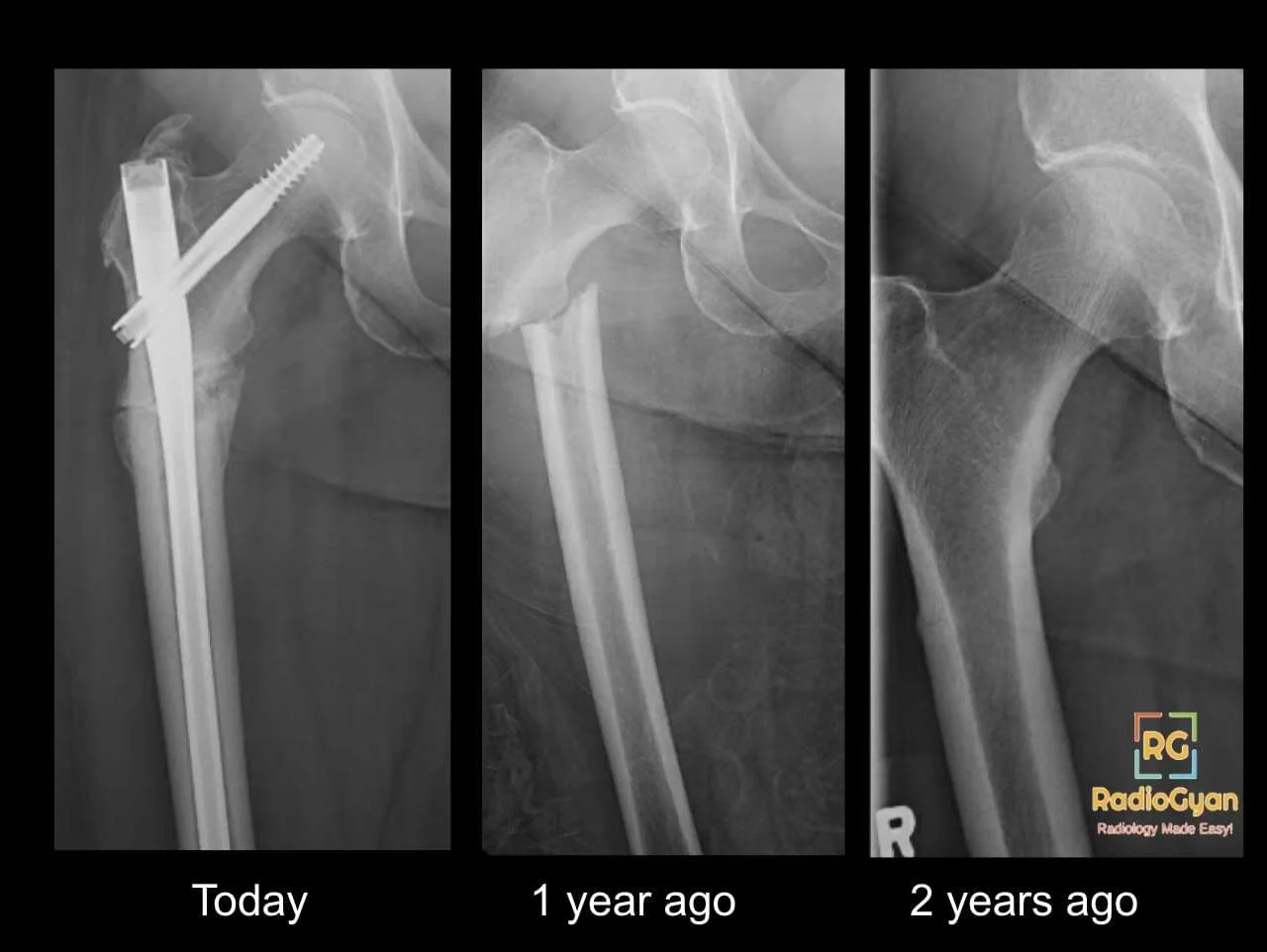
Read this detailed article on atypical femoral fractures to understand why a radiologists role is important in diagnosing these:
Imaging:
Radiographs may not always show nondisplaced fractures, especially in osteoporotic patients. In these cases, noncontrast MRI is recommended.
CT of the abdomen and pelvis obtained for trauma evaluation can often show unsuspected femoral neck fractures.
MRI findings include a hypointense fracture line and band-like marrow edema on T1WI and high-signal bone marrow edema on T2WI FS/STIR sequences.

Differential diagnoses for femoral neck fractures include femoral head fractures, intertrochanteric fractures, osteoarthritis, transient bone marrow edema syndrome, and muscle tears.
Key teaching points:
- The lateral margin of the femoral head-neck junction is crucial because this is the most common penetration point of the lateral epiphyseal vessels, and fractures involving this area create a high risk of critical vascular injury, with generally decreasing risk as fractures occur more distally along the femoral neck.
- Valgus-impacted fractures are frequently missed on initial radiographs owing to the subtlety of cortical distortion at the femoral head-neck junction and relatively mild fracture angulation, and they are often apparent only on the basis of the presence of a characteristic sclerotic lateral cortical impaction triangle.
- Isolated fractures of the lesser trochanter in adults should be considered pathognomonic for tumor infiltration, due to the relative rarity of traumatic avulsions in this population compared with children.
Treatment options for femoral neck fractures depend on the type and displacement of the fracture and may include percutaneous pinning, dynamic hip screw, cephalomedullary nail, ORIF, hemiarthroplasty, or total hip arthroplasty.
MCQ question: What imaging modality is recommended if radiographs are negative or equivocal for femoral neck fracture in osteoporotic patients?
a) CT scan
b) MRI
c) Bone scan
d) Ultrasound
Single best reference article:
Illustrations by TeamGyan Member Dr. Disha Lokhandwala.


Wow, this article breaks down hip fractures super clearly! The bit about intracapsular vs extracapsular and AVN risk makes total sense now. Definitely saving this for reference. Great job explaining complex anatomy simply.
Thank you for your kind words.