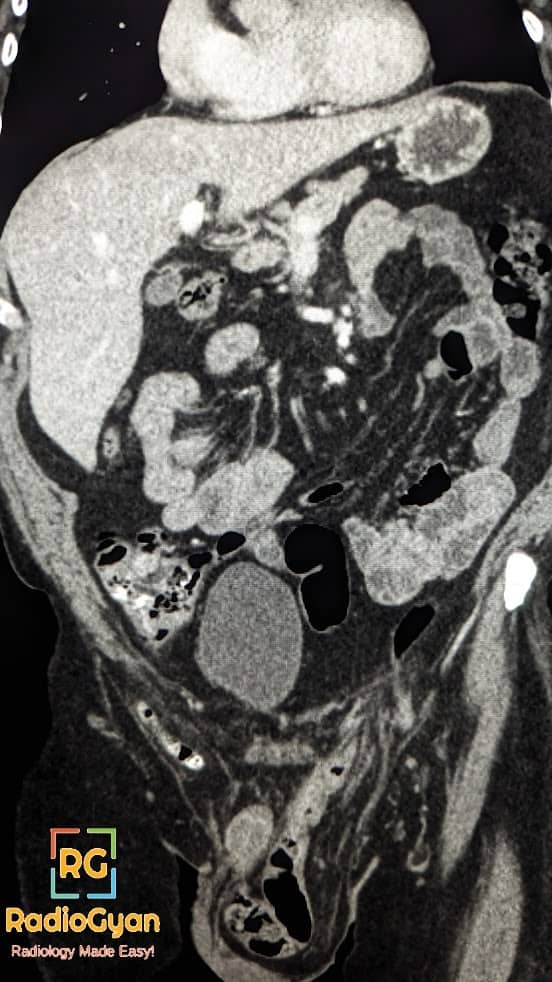
Amyand hernia is a rare type of inguinal hernia where the appendix is found within the hernia sac.
Etymology
It is named after the English surgeon Claudius Amyand, who first described it in 1735.
Clinical Features
It can be either congenital or acquired. Amyand’s hernia is 3 times more likely to be diagnosed in children than in adults, due to a patent processus vaginalis in the pediatric population. It is seen almost exclusively in males and rarely in postmenopausal patients. It is mostly asymptomatic.
The incidence of acute appendicitis in Amyand hernia is 0.1%. Complications are similar to those seen in acute appendicitis and include perforation, abscess formation, strangulation and incarceration.
Although very rare, LEFT sided Amyand hernia can be seen in patients with situs inversus, intestinal malrotation, or with a mobile cecum.
Imaging
Imaging features of an Amyand hernia include a blind-ending tubular structure arising from the cecum and extending into the inguinal sac, with or without inflammatory changes.
Management
Treatment for Amyand’s hernia is appendectomy via herniotomy, with primary hernia repair . Laparoscopic appendicectomy has been increasingly performed recently.
Other eponymous/named hernias:
| Bochdalek’s Hernia | Congenital Posterolateral Hernia of Diaphargm |
| Morgagni Hernia4 | Through Larry’s space in Diaphargm |
| Larry’s Hernia4 | |
| Gibbon Hernia | Hernia with Hydrocele |
| Bergers Hernia | Hernia in Pouch of Douglas |
| Romberg Hernia1 | Concurrent Ipsilateral Direct and indirect Inguinal Hernia |
| Saddle Hernia1 | |
| Dual Hernia1 | |
| Lumbar Hernia | Hernia in lumbar triangles of type Petit’s and Grynfelt |
| Obturator Hernia | Hernia through Obturator Canal |
| Grynfelt Hernia | Upper Lumbar triangle Hernia |
| Petit’s Hernia | Lower Lumbar Triangle Hernia |
| Femoral Hernia | Hernia medial to Femoral Vein in Femoral canal |
| Cooper’s Hernia6 | Femoral Hernia with two sacs |
| Bilocular femoral Hernia6 | |
| Cloquet’s Hernia | Hernia Through Pectineal aponeurosis |
| Callison-Cloquet Hernia | Through Pectineus Muscle and its fascia |
| Narath’s Hernia | Behind Femoral Artery in congenital dislocation of Hip |
| Hesselbach’s Hernia | Lateral to Femoral Artery |
| Serofini’s Hernia | Behind Femoral Vessels |
| Laugier’s Hernia | Through Lacunar Ligament |
| Teale’s Hernia5 | In front of Femoral Vessels |
| Velpeau Hernia5 | |
| Richter’s Hernia | Part of circumference of bowel wall is entrapped |
| Littre’s Hernia | Contains Meckel Diverticulum |
| Sliding Hernia | Hernia with a part of the wall formed by the viscus |
| Hernia En Glissae | Hernia with a part of the wall formed by the viscus |
| Maydl’s Hernia2 | Two loops of bowel in Hernia sac with remaining part in abdomen |
| W Hernia/Hernia in W2 | |
| Retrograde Hernia2 | Two loops of bowel in Hernia sac with remaining part in abdomen |
| Phantom Hernia | Localised Muscle Bulge following Muscle Paralysis |
| Mery’s Hernia7 | Through the perineal floor |
| Perineal Hernia7 | |
| Spigelian Hernia | Hernia through Speligian Fascia |
| Sciatic hernia | Hernia through greater or lesser sciatic foramen |
| Little’s hernia3 | Appendix in inguinal Hernial Sac |
| Amyand hernia3 | |
| De Garengeots Hernia | Incarceration of appendix within Femoral Hernia |
| Beclards Hernia | Femoral Hernia Through Saphenous Opening |
| Barth’s Hernia | Hernia Between Adbominal wall and Persistent Vitellointestinal Duct |
| Holthouse’s Hernia | Inguinal Hernia That has turned outward into the groin |
| Grubers Hernia | Internal Mesogastric Hernia |
| Mesocolic hernia | Transmesenteric Hernia |
| Kronlem Hernia | Inguinoproperitoneal Hernia |
| Trietz Hernia | Paraduodenal Hernia |
| Rieux Hernia | Retrocaecal Hernia |
Single Best Reference Article: