Key Takeaways
| ASPECTS Score | Importance |
|---|---|
| Alberta Stroke Program Early CT Score (ASPECTS) | A 10-point quantitative topographic computed tomography scan score used in predicting functional outcomes and symptomatic hemorrhage. |
| Clinical Use | Used to assess the extent of early ischemic changes on computed tomography (CT) scans in the middle cerebral artery territory. |
| Thrombolysis | ASPECTS score is used to predict the outcomes of thrombolysis treatment. |
Introduction to ASPECTS Score
The Alberta Stroke Program Early CT Score (ASPECTS) is a 10-point quantitative topographic computed tomography (CT) scan score used in predicting functional outcomes and symptomatic hemorrhage. It was developed to offer a reliable and reproducible method of assessing the extent of early ischemic changes on computed tomography (CT) scans in the middle cerebral artery territory.
ASPECTS is a crucial tool in neuroradiology, providing valuable information that can guide treatment decisions and predict patient outcomes. Its use has been widely adopted in clinical practice, and it continues to be a subject of ongoing research.
History of ASPECTS Score
The ASPECTS score was first introduced by a group of researchers at the University of Calgary, Canada. Recognizing the need for a standardized method to quantify early ischemic changes on CT scans, they developed the ASPECTS score as a simple yet effective tool.
Since its introduction, the ASPECTS score has undergone several revisions and updates to improve its accuracy and applicability. Today, it is recognized globally as an essential tool in the field of neuroradiology.
Understanding the Scoring System
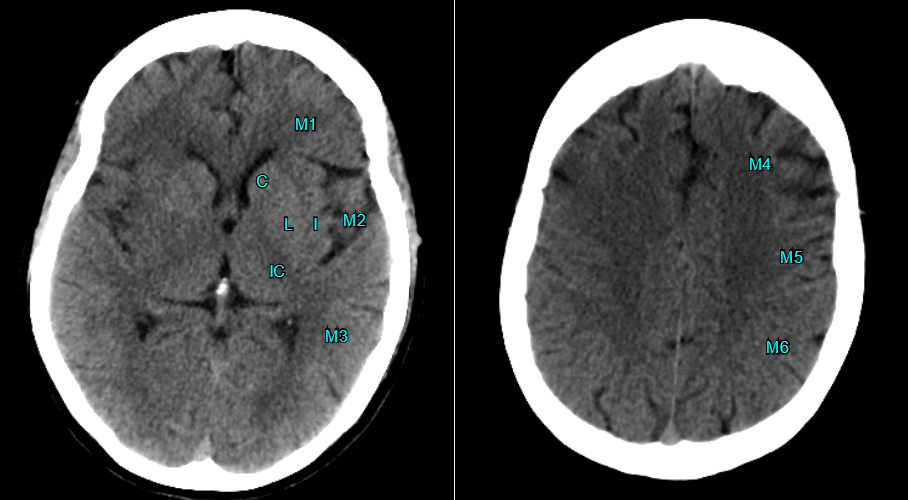
The ASPECTS scoring system is based on a 10-point scale that assesses specific regions of the brain affected by ischemia. The regions evaluated include the caudate, lentiform, internal capsule, insular ribbon, M1, M2, M3, M4, M5, and M6 segments.
Each region is assigned a score from 0 to 1. A score of 1 indicates no early ischemic change, while a score of 0 indicates early ischemic change. The scores for all regions are then summed to give a total ASPECTS score. A lower total score indicates more extensive early ischemic changes.
Clinical Use of ASPECTS Score
In clinical practice, the ASPECTS score is used to assess patients who have suffered an acute ischemic stroke. By providing a quantitative measure of early ischemic changes on CT scans, it helps clinicians predict functional outcomes and symptomatic hemorrhage.
The ASPECTS score also plays a crucial role in guiding treatment decisions. For example, it can help determine whether a patient is a suitable candidate for thrombolytic therapy or endovascular treatment.
ASPECTS Score and Thrombolysis
Thrombolysis is a treatment that dissolves blood clots and restores blood flow to the brain. The success of this treatment largely depends on the extent of early ischemic changes, which can be quantified using the ASPECTS score.
Studies have shown that patients with a high ASPECTS score (indicating fewer early ischemic changes) are more likely to benefit from thrombolysis. On the other hand, patients with a low ASPECTS score may be at higher risk for symptomatic hemorrhage following thrombolysis.
Posterior Circulation ASPECTS (pc-ASPECTS)
While the original ASPECTS score was designed for the anterior circulation, a modified version known as the Posterior Circulation Alberta Stroke Program Early CT Score (pc-ASPECTS) has been developed for the posterior circulation. This scoring system assesses ten anatomical regions within the posterior circulation, including the thalamus, midbrain, pons, medulla, and cerebellum.
Just like the original ASPECTS score, each region in pc-ASPECTS is assigned a score of 0 or 1, with a lower total score indicating more extensive ischemic changes. This allows for a more comprehensive assessment of stroke patients and helps guide treatment decisions in cases of posterior circulation stroke.
Case Studies Illustrating ASPECTS Score Application
To illustrate the application of the ASPECTS score in clinical practice, let’s consider two hypothetical case studies:
- Case Study 1: A 65-year-old patient presents with acute onset of right-sided weakness and speech difficulty. A CT scan reveals early ischemic changes in the left MCA territory. The patient’s ASPECTS score is calculated as 7, indicating moderate early ischemic changes. Based on this score, the patient is considered a suitable candidate for thrombolysis.
- Case Study 2: A 70-year-old patient presents with acute onset of left-sided weakness and visual disturbance. A CT scan reveals extensive early ischemic changes in the right MCA and PCA territories. The patient’s ASPECTS score is calculated as 3, indicating severe early ischemic changes. Based on this score, the risks of thrombolysis may outweigh the benefits for this patient.
These case studies highlight how the ASPECTS score can be used to guide treatment decisions and predict outcomes in stroke patients.
Limitations and Challenges of ASPECTS Score
Despite its usefulness, the ASPECTS score is not without limitations. One of the main challenges is that it requires a certain level of expertise to accurately assess early ischemic changes on CT scans. This can lead to variability in scoring between different observers.
Furthermore, the ASPECTS score only assesses early ischemic changes in the MCA territory (or posterior circulation in the case of pc-ASPECTS). It does not take into account other factors that may influence patient outcomes, such as age, comorbidities, or time from symptom onset to treatment.
Despite these limitations, the ASPECTS score remains a valuable tool in neuroradiology. Ongoing research and development are expected to further improve its accuracy and applicability.
Future Directions for ASPECTS Score Research
The ASPECTS score has proven to be a valuable tool in neuroradiology, but there is always room for improvement. Future research could focus on several areas to enhance its utility and accuracy.
One potential area of research is the development of automated scoring systems. These could use machine learning algorithms to automatically calculate the ASPECTS score from CT scans, reducing the potential for human error and variability between observers.
Another area of interest could be the incorporation of additional clinical factors into the scoring system. For example, patient age, time from symptom onset to treatment, and presence of comorbidities could all influence patient outcomes and may be worth considering in the ASPECTS score.
Finally, more research is needed to validate and refine the pc-ASPECTS score for posterior circulation strokes. This could involve large-scale studies comparing the predictive accuracy of pc-ASPECTS with other scoring systems.
Conclusion
The Alberta Stroke Program Early CT Score (ASPECTS) is a crucial tool in neuroradiology, providing a quantitative measure of early ischemic changes on CT scans. It guides treatment decisions, predicts patient outcomes, and has been widely adopted in clinical practice.
Despite its limitations, ongoing research and development are expected to further improve its accuracy and applicability. As our understanding of stroke pathology continues to evolve, so too will our tools for assessing and treating this devastating condition.
In conclusion, whether you’re a seasoned neuroradiologist or a radiology resident just starting out, understanding and correctly applying the ASPECTS score is an essential skill in stroke management.
What does ASPECTS stand for?
ASPECTs stands for Alberta Stroke Program Early CT Score.
What is the ASPECTS in stroke?
Alberta Stroke Program Early CT score (ASPECTS) is a 10-point quantitative score used to assess early ischemic changes on non-contrast CT head studies.
What is the clinical significance of the ASPECTS / How to interpret the ASPECT Score?
- Reliable and reproducible grading system on non-contrast CT examinations of the head for detection of early ischemic changes in patients suspected of having acute large anterior circulation occlusion.
- It is used as part of the assessment for eligibility in receiving interventional mechanical thrombectomy treatment.
- It quantifies CT changes in early middle cerebral artery stroke. A lower score suggests poorer outcome.
- Patients with scores ≥8 have a higher chance for an independent outcome.
- Patients with ASPECTS 0–4 had significantly worse outcome than patients with ASPECTS 5–10 and did not benefit from faster treatment, thus suggesting a cutoff ASPECTS ≤4 to identify patients with poor response to intravascular treatment.
What is normal ASPECTS score?
An ideal ASPECTS score is 10 when none of the vital structures are involved by acute ischemic changes. But patients with scores ≥8 have a higher chance for an independent outcome.
What are the anatomical regions used to assess acute stroke in ASPECTS?
The template consists of 10 anatomically defined regions.
- Subcortical : 4 subcortical structures [caudate (C); lentiform (L); internal capsule (IC); insular ribbon (I)]
- Cortical : 6 for cortical structures in the MCA territory, labeled M1–M6.
- Ganglionic : On the level of the caudate head or below are hereby allotted to the ganglionic level,
- Supraganglionic : Above the level of the caudate head.
How are ASPECT scores calculated?
For each ASPECTS region that presents with early ischemic changes with loss of gray-white differentiation on at least two consecutive cuts, the overall score of 10 is reduced by 1.
What are the recommended window settings for calculating ASPECTS?
Ideal window settings for calculating ASPECTS are window level of 30 H with a window width of 80 H.
What are the pitfalls while calculating ASPECTS?
- Motion artifacts.
- Atrophy, white matter ischemic changes (leucoaraiosis) and old infarcts need to be properly evaluated.
What is DWI-ASPECTS?
ASPECTS can be used to assess extent of infarction on DWI images and is termed as DWI-ASPECTS. DWI-ASPECTS within 3 h after symptom onset has been proven to predict functional outcome (Modified Rankin Scale, MRS) and mortality after 3 months in patients undergoing IV-thrombolysis.
- DWI-ASPECTS >5 within 3 h after onset : Good functional outcome 7 days after IV-thrombolysis.
- DWI-ASPECTS >7 from 3-24h after onset: Good functional out come in 3 months (MRS ≥3).
What is pc-ASPECTS?
pc- ASPECTS stands for Posterior Circulation ASPECTS and is a similar scale for evaluation of posterior circulation. Points are subtracted from 10 as follows:
- Thalami (1 point each)
- Occipital lobes (1 point each)
- Midbrain (2 points)
- Pons (2 points)
- Cerebellar hemispheres (1 point each)
Further reading and resources:
- ASPECTS
- Use of the Alberta Stroke Program Early CT Score (ASPECTS) for Assessing CT Scans in Patients with Acute Stroke
- A Critical Review of Alberta Stroke Program Early CT Score for Evaluation of Acute Stroke Imaging

About the Author
Dr. Amar Udare, MD, DNB
Dr. Udare holds an MBBS and MD degree, and his expertise lies in the field of radiology. He has authored multiple peer-reviewed publications, contributing significantly to the medical field. His works can be accessed on PubMed and Google Scholar.
In addition to his academic and professional achievements, Dr. Udare is an avid reader and enjoys exploring the latest advancements in medical technology. His commitment to making complex medical knowledge accessible to patients and the general public aligns with our mission at RadioGyan.com.
For any further questions or clarifications, feel free to reach out to Dr. Udare via the contact form.